Feature Story
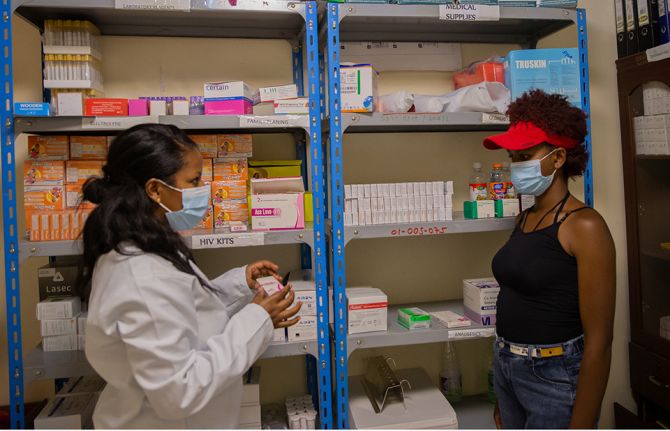
Protecting the confidentiality and security of personal health information
23 November 2016
23 November 2016 23 November 2016Health services are being scaled up in many low- and middle-income countries. This has resulted in a substantial increase in the amount of personal health information collected in order to develop and maintain comprehensive health records of a person’s use of the services and to monitor and evaluate the use, cost, outcomes and impacts of programmes or services. Detailed personal health information is also needed to evaluate success towards achieving, for example, the 90–90–90 targets, universal health coverage and the Sustainable Development Goals.
However, if personal health information is not held confidentially and securely, people may be reluctant to use health services, owing to fear of being stigmatized or discriminated against. The confidentiality and security of personally identifiable information therefore has to be protected at all levels of the health system. In many countries, this will require the development and implementation of privacy laws and a confidentiality and security framework for protecting personal health information.
Based on the principles of privacy, confidentiality and security, UNAIDS and PEPFAR have developed an assessment tool and an user manual to support countries to assess the degree that the confidentiality and security of personal health information is protected at facility and data warehouse levels and whether national guidelines that include privacy laws exist.
Many countries are in the process of developing and implementing national health identifiers (NHIDs) to ensure that each patient has a unique identity within the health system. This facilitates the development of comprehensive medical records and allows users of services to be tracked across health-care sectors. The development and use of NHIDs in a country’s health-care system promotes the effectiveness and efficiency of data gathering, but their use further underlines the need to protect the confidentiality and security of personal health information.
While policy-makers and other stakeholders in several countries recognize the need to develop and implement policies for protecting the privacy, confidentiality and security of personal health information, to date few countries have developed, let alone implemented, such policies. A workbook has also been developed that can be used to perform the actual assessments in country to assess to what extent policies have been developed and implemented at facility, data warehouse and national levels.
Privacy, Confidentiality and Security Assessment Tool
Related




Feature Story
Sex Workers Academy Africa: increasing demand for rights-based HIV prevention services
21 November 2016
21 November 2016 21 November 2016The Sex Worker Academy Africa is a ground-breaking learning programme that aims to strengthen the rights of sex workers across 47 countries in Africa. It focuses on rapidly scaling up sex worker-led responses to HIV, increasing demand for and access to high-quality rights-based HIV prevention and treatment services for female, male and transgender sex workers and increasing HIV testing, leading ultimately to a fall in new HIV infections among sex workers.
The academy’s curriculum is based on the Sex Worker Implementation Tool. Developed by UNAIDS and partners in 2013, the tool outlines recommendations for the prevention and treatment of HIV and other sexually transmitted infections among sex workers in low- and middle-income countries.
Launched in 2015 and since held several times a year, the academy brings together sex workers from across the continent to explore issues such as community empowerment, addressing violence against sex workers, condom and lubricant programming, community-led services and capacity-building. The curriculum includes knowledge-sharing, art and dance advocacy projects, site visits, thematic workshops and feedback sessions. Each academy lasts a week and includes up to 18 participants.
Since its launch, more than 130 sex workers from 17 African countries have graduated from the academy. It has enabled sex workers from Namibia, the United Republic of Tanzania, Zambia and Zimbabwe to form their own national sex worker networks. In addition, sex workers from Lesotho and Swaziland have organized grass-roots organizations for sex workers where previously none had existed.
The academy is an African Sex Workers Alliance initiative implemented by the Kenya Sex Workers Alliance in Nairobi, Kenya. The curriculum was developed in cooperation with the Ashodaya Academy and the VAMP Institute in India, the Asia Pacific Network of Sex Workers and the Global Network of Sex Workers.
Initial funding for the development of the academy was provided by the United Nations Population Fund and the Dutch-funded nongovernmental organization Bridging the Gaps. Bridging the Gaps and the Robert Carr Fund have provided funding for the ongoing implementation of the academy’s work.
HANDS UP FOR #HIVPREVENTION — WORLD AIDS DAY CAMPAIGN


Feature Story
HIV prevention among key populations
22 November 2016
22 November 2016 22 November 2016Since 2010, the annual global number of new HIV infections among adults (15 years and older) has remained static, at an estimated 1.9 million. Members of key populations, including sex workers, people who inject drugs, transgender people, prisoners and gay men and other men who have sex with men, and their sexual partners accounted for 45% of all new HIV infections in 2015.
In some countries and regions, infection rates among key populations are extremely high—HIV prevalence among sex workers varies between 50% and 70% in several countries in southern Africa. One study from Zimbabwe found HIV prevalence rates of 27% for male inmates, 39% for female inmates and 60% for sex workers, with 9.6% of these getting newly infected between 2009-2014. New infections among gay men and other men who have sex with men have been increasing in all regions in recent years. Across countries, key populations are between 10 and 50 times in greater risk of HIV infection compared to other adults.
Criminalization and stigmatization of same-sex relationships, sex work and drug possession and use, and discrimination, including in the health sector, are preventing key populations from accessing HIV prevention services. Effective government support and community-based and implemented HIV prevention and treatment programmes that provide tailored services for each group are currently too few and too small to result in a significant reduction in new infections.
In order to achieve the target of reducing new HIV infections among key populations by 75% by 2020, a large-scale increase of programmes and the creation of an enabling social and legal environment are needed.
We must reduce new HIV infections among key populations
The global number of new HIV infections among adults has remained static, at an estimated 1.9 million, since 2010, threatening further progress towards the end of the AIDS epidemic.
New HIV infections among gay men and other men who have sex with men are rising globally, and there has been no apparent reductions of new infections among sex workers, transgender people, people who use drugs or prisoners. Studies conducted in southern Africa have found HIV prevalence 10–20 times higher among sex workers than among adults in the general population, with rates of HIV infection reaching 50% of all sex workers tested, and HIV prevalence reaching 86% in one study in Zimbabwe. A synthesis of studies including more than 11 000 transgender people worldwide estimates HIV prevalence to be 19.1%.
Key populations remain among the most vulnerable to HIV. Analysis of the data available to UNAIDS suggests that more than 90% of new HIV infections in central Asia, Europe, North America, the Middle East and North Africa in 2014 were among people from key populations and their sexual partners, who accounted for 45% of new HIV infections worldwide in 2015.
Reinvigorating HIV prevention among key populations requires domestic and international investments to provide key populations with tools, such as condoms and lubricants, pre-exposure prophylaxis and sterile needles and syringes, and testing and treatment. However, the design and delivery of such HIV combination prevention services is often limited by a reluctance to invest in the health of key populations and to reach out to them.
In many countries, key populations are pushed to the fringes of society by stigma and the criminalization of same-sex relationships, drug use and sex work. Marginalization, including discrimination in the health sector, limits access to effective HIV services. There is an urgent need to ensure that key populations are fully included in AIDS responses and that services are made available to them.
Guidelines and tools have been developed for and with the participation of key populations in order to strengthen community empowerment and improve the delivery of combination prevention services by community-led civil society organizations, governments and development partners.
The available evidence shows that when services are made available within an environment free of stigma and discrimination and involving key population communities, new HIV infections have declined significantly. For example, street youth in St Petersburg had a 73% decrease in HIV seroprevalence from 2006 to 2012, primarily due to decreased initiation of injection drug use. This marked reduction in the HIV epidemic among street youth occurred after implementation of extensive support programs and socio-economic improvements.
The replication of such successes and the scale-up of combination prevention programmes in all cities and sites where key populations live and work, implemented by countries and community organization networks, will help prevention efforts get back on track to achieving the target of reducing new HIV infections by 75% by 2020.
Quotes
“WHAT MATTERS IS THE LACK OF INCLUSION AND WIDESPREAD DISCRIMINATION. IT IS CLEAR THAT WE CANNOT END THE AIDS EPIDEMIC WITHOUT TAKING CARE OF THE NEEDS OF KEY POPULATIONS.”
Hands up for #HIVprevention — World AIDS Day campaign



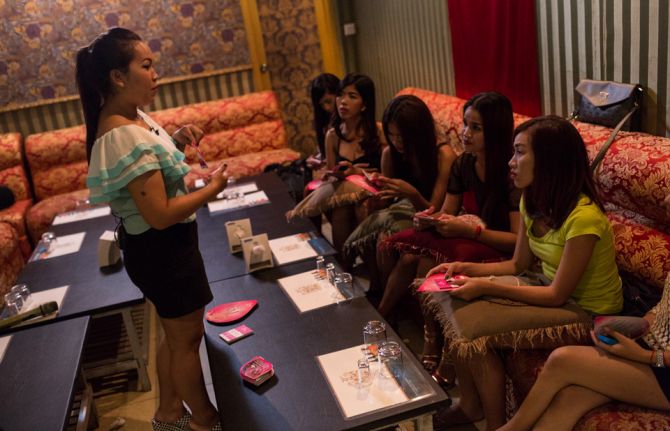

Feature Story
Bringing HIV testing to communities in Cambodia
15 November 2016
15 November 2016 15 November 2016It is nine o’clock in the evening and the night is just beginning in one popular area of Phnom Penh, Cambodia. One multistorey building offers a range of entertainment options: diners enjoy a meal on the ground floor, the bars in the middle level vibrate with popular songs and on the top floor is a hotel.
However, in one corner, next to several karaoke rooms, a serious conversation is taking place. It seems out of context amid the high-pitched laughter, strobe lights, brightly dressed women and male customers. Five entertainment workers are sitting on a sofa talking about why they don’t get tested for HIV.
One woman said, “I don’t know where to go.”
A co-worker agreed and added, “I daren’t go. I am too afraid.”
Their interviewer is 22-year-old Rath Chan Molika. She recently quit her job as an entertainment worker and is now an outreach worker and counsellor with the SMARTgirl programme. She explained why the women working in the karaoke parlour feared public health clinics. “First of all, it’s because they’re scared to go alone,” she says. “Secondly, they’re afraid of the needle and blood.”
There were an estimated 34 000 entertainment workers in Cambodia in 2015, meeting clients in hotels, karaoke parlours, beer gardens, casinos and massage parlours. Unprotected sexual relations with male customers can place some women at higher risk of HIV.
“Some go out with customers without using a condom correctly and consistently. And sometimes they use drugs together, sharing needles and syringes, which increases their risk of HIV,” said Ms Molika.
As part of her job with the SMARTgirl programme, she informs entertainment workers about how to protect themselves from HIV and other sexually transmitted infections and unintended pregnancy. While HIV peer counselling in entertainment establishments has been conducted for a few years, Ms Molika is participating in a highly innovative HIV testing programme.
When the group counselling session ends, she breaks away and in a separate room welcomes Mao Soma. The two women chat quietly for a moment. Ms Molika has been trained to provide pre- and post-HIV-test counselling and to conduct a rapid finger prick test. While Ms Soma winces as the needle pricks her finger, the procedure is over before long. Within 15 minutes there is a result, which suits Ms Soma. “The test is quick and I can get the result immediately,” she says.
Cambodia’s AIDS epidemic is concentrated in key populations
As in many other countries in the region, Cambodia’s AIDS epidemic is concentrated in key populations at higher risk of HIV, which includes entertainment workers, gay men and other men who have sex with men, transgender people and people who inject drugs.
“The government of Cambodia gives importance to collaboration with civil society and also with local people at the community level,” says Ieng Mouly, the Chair of the National AIDS Authority.
Technological innovation in HIV testing
The government, civil society partners and international organizations are now promoting rapid finger prick testing for key populations to replace traditional tests that require laboratory analysis.
“Bringing the facility close to the people is always best. People don’t have to depend on sophisticated laboratory equipment,” explains Ly Penh Sun, the Director of the National Centre for HIV/AIDS, Dermatology and STD.
“The people who are conducting the tests are familiar with the people they are testing. They can interact more. They can support each other,” says Choub Sok Chamreun, of the nongovernmental organization Khana, which provides HIV prevention, care and support services at the community level.
The need for community-based approaches
This community-based HIV testing programme is one of the first of its kind in the Asia and the Pacific region. Across the region, HIV testing coverage among key populations is low. While many countries have scaled up HIV testing in health clinics, representatives of civil society have called for more community-based approaches, focusing on key populations, who often do not attend health clinics.
The results from the Cambodian model are encouraging. Over the past year, implementers reported that more than 36 000 people from key populations were tested, 80% more than in 2014. If a person has a positive reaction on a first rapid screening test, they are accompanied by outreach workers to health facilities for confirmatory tests. Once a medical professional confirms the result, the person has access to HIV treatment.
To improve their efforts to find more people living with HIV, implementation partners are retooling the programme to intensify outreach to people at the highest risk within each key population.
“The plan is to modify the outreach guidelines to the populations at highest risk and intensify targeted outreach activity, as well as active case management, to register and retain the people who were found to be HIV-positive, to ensure they receive treatment,” says Mr Sun.
Hands up for #HIVprevention — World AIDS Day campaign
Region/country
Related


Feature Story
Reducing the impact of HIV among adolescent girls
11 November 2016
11 November 2016 11 November 2016Around 180 young women and adolescent girls from Malawi, Kenya and Uganda have led a pilot project that aims to strengthen the leadership of young women and adolescent girls in the AIDS response. Called Empowerment + Engagement = Equality, the programme aims to build stronger leadership among young women and adolescent girls to engage in national assessments initiated by the All In to #EndAdolescentAIDS platform. The programme addresses issues of gender inequality that heighten adolescent girls’ vulnerability to HIV infection and provides safe spaces where experiences can be shared.
The initiative, designed and implemented by UN Women and the International Planned Parenthood Federation, mobilized more than 1000 young advocates, including young women living with HIV, to voice their concerns at the local, regional and national levels. As well as sharing knowledge among themselves, the participants engaged in face-to-face and online meetings with parents, teachers, religious leaders and other community stakeholders to discuss how to change harmful gender norms and inequalities that increase the risk of HIV infection.
The First Lady of Malawi, Gertrude Mutharik, participated in one of the discussions and committed her support to challenging the issues that increase the risk of HIV infection among young women, including gender-based violence. The young leaders have continued to advocate at the highest levels, taking part in debates at the International AIDS Conference in Durban, South Africa, in July 2016.
“Some of the most fulfilling work I have done as part of this project is to support other girls like me to feel empowered and in control of their lives,” said Divina Kemunto, from Kenya, “I shared my personal experience and encouraged girls living with HIV to believe that they too can walk with their heads held high and a smile on their face.”
Preventing new HIV infections among adolescent girls and young women in sub-Saharan Africa is crucial if the world is to end the AIDS epidemic by 2030—in 2015, 75% of new HIV infections in sub-Saharan Africa among adolescents were among adolescent girls aged 10–19 years. Preventing infections means empowering young women and girls to stay in school so they have better economic prospects, ensuring that they have the knowledge, information and tools to avoid unintended pregnancy and sexually transmitted infections and making sure they know what to do when faced with sexual violence.
Laws and policies that discriminate against women and girls must be dismantled and their sexual and reproductive health and rights must be fully respected.
Hands up for #HIVprevention — World AIDS Day campaign


Feature Story
How one Jamaican organization is empowering adolescent girls living with HIV
10 November 2016
10 November 2016 10 November 2016Rushell Gray unflinchingly shares the story of her journey to the edge and back. She was infected with HIV after being abused at the age of nine, but her eight-year-old daughter is HIV-free. “It has been difficult. As a young girl in the community everybody turned a blind eye and blamed me,” she said. “Nobody said this man needs to go to jail. At one point I gave up because the stress was too high,” she recounts.
A petite young woman, Ms Gray is confident and articulate. She credits the Jamaican nongovernmental organization Eve for Life and its transformative programme for her turnaround. Through a combination of counselling, personal development and life-skills education, she has become one of the powerhouse peer educators of Mentor Moms.
The Mentor Moms programme deploys young, empowered women who are affected by HIV and young mothers to help others along the journey. They answer questions and offer reassurance, accompany adolescent girls to their clinic visits and they reinforce guidance on taking medicines, avoiding breastfeeding and keeping clinic appointments.
Ms Gray clarifies that the issues her mentees face are not just about HIV. “They do not have resources, they are not safe in their houses, they are afraid a partner or their family might throw them out. They might have two children or more,” she said. A 2012 survey by the Jamaica National HIV/STI Programme found that one in every five adolescent girls in Jamaica aged 15–19 years reported having experienced sexual violence.
Eve for Life Executive Director and co-founder Patricia Watson noted that many girls are being left behind. “A recent study showed that among girls in state care, 30% have sexually transmitted infections, 41% attempted suicide and 35% have been forced to have sex. Also, children infected with HIV at birth are growing older and becoming sexually active, some without having been informed about their status,” she said.
For the organization, responding to HIV among adolescent girls is about far more than promoting sex messages. It is fundamentally about social protection and addressing the structural and social issues that increase girls’ vulnerability.
For the past two years, Eve for Life has spearheaded the Nuh Guh Deh! (Don’t Go There) national campaign to end sex with girls.
“The overarching goal is to contribute to reducing sexual abuse of girls in Jamaica,” Ms Watson said.
The campaign seeks to mobilize Jamaicans to report acts of sexual violence while increasing awareness about the long-term effects of abuse and the links to HIV. Survivor stories highlight the serious issues they face. The approach maximizes participation and ownership from adolescent girls and young women who have survived sexual abuse.
The Nuh Guh Deh song by the Jamaica dub poetry group No-Maddz aims to reduce social acceptance of predatory relationships between older men and girls.
Hands up for #HIVprevention — World AIDS Day campaign
Region/country
Related


Feature Story
#WhatWomenWant for the HIV response: a new space for new conversations
10 November 2016
10 November 2016 10 November 2016#WhatWomenWant is a virtual space that amplifies the voices of young women, allowing them to share expertise and life experiences, explore solutions and build strengthened networks across gender-related issues, sectors and movements.
Inspired by the impact of the virtual activism surrounding the 2016 Commission on the Status of Women, the Athena Network and its partners, including UNAIDS, used the momentum to build a platform where women could mobilize around the United Nations General Assembly High-Level Meeting on Ending AIDS. From May to July 2016, a social media campaign reached 13 million Twitter accounts and organized five Twitter conversations that engaged 120 000 people. The aim was to hear what women want and to identify specific actions needed to change the lives of women and girls.
The initiative continues to engage an expanding network of primarily women-led organizations working to advance gender equality, with a special focus on areas where health and rights meet.
#WhatWomenWant aims to:
- Focus attention on the urgent need to address women’s rights and gender-related disparities within and beyond the HIV response.
- Act as a catalyst for joined-up action where gender equality, human rights, sexual and reproductive health issues, gender-based violence and the HIV response intersect.
- Put women in charge of defining their own agendas.
- Harness the experience of women to create advocacy tools to advance their own solutions wherever they are.
- Identify opportunities for women to engage stakeholders and to be meaningfully involved in the decision-making processes that most affect their lives.
#WhatWomenWant continues to strengthen links across movements to end child marriage, stop sexual violence, ensure safe and legal abortion rights and advance comprehensive sexuality education.
“At a time when funding for women's rights has been on the decline, the #WhatWomenWant online campaign provides a space for young feminists to contribute to and influence global policy discussions on the HIV response,” says Catherine Nyamburra, a young activist from Kenya. “It provides a space to amplify young feminist voices through various channels of participation and for feminist thought leadership in the response to HIV.”
Video
United States Global AIDS Ambassador, Deborah Birx, explains why young women are more vulnerable to becoming infected with HIV. 1000 young women are being infected every day = 7000 a week globally.
Hands up for #HIVprevention — World AIDS Day campaign
Campaigns




Feature Story
Comprehensive sexuality education in Zambia
09 November 2016
09 November 2016 09 November 2016It is estimated that worldwide only three in 10 adolescent girls and young women between the ages of 15 and 24 years have comprehensive and correct knowledge about HIV.
With inadequate knowledge, young people are ill-equipped to make healthy and safe decisions about their sexual health. However, knowledge, while a crucial foundation, is not in itself sufficient to change behaviour and reduce the risk of HIV infection. Knowledge needs to be combined with the right skills and attitudes, which can be taught and developed through high-quality comprehensive sexuality education (CSE).
CSE not only plays an important role in preventing negative sexual and reproductive health outcomes, but also offers a platform to discuss gender issues and human rights and to promote respectful, non-violent relationships. However, gender-responsive and life-skills-based HIV and sexuality education is only covered in the national curriculum by 15% of the 78 countries analysed in the Global education monitoring report, recently launched by the United Nations Educational, Scientific and Cultural Organization.
When CSE programmes focus on gender and power relations, they are much more likely to show positive effects in reducing sexually transmitted infections and unintended pregnancies than programmes ignoring gender and power.
Such a gender-responsive CSE programme have been implemented in Zambia, which is a signatory to the 2013 Ministerial Commitment on comprehensive sexuality education and sexual and reproductive health services for adolescents and young people in eastern and southern Africa.
The curriculum in Zambia focuses on puberty, HIV prevention, gender equality, sexual and reproductive health, relationships and human rights. The overall goal is for adolescents and young people in Zambia to enjoy better sexual and reproductive health and have better health outcomes overall.
Zambia currently has the largest population of young people in its history, with 52.5% aged below 18 years. During their school years, teachers and sexual health specialists have an ideal opportunity to reach students with correct and appropriate health education information. The onset of adolescence brings not only physical change but also vulnerabilities to human rights abuses, particularly in the areas of sexuality, marriage and childbearing.
Harriet Lilanda, aged 13, a student at Twalumba Primary School in Lusaka, Zambia, thinks that the new sexuality education curriculum is important for young people. “Talking openly about sexuality was not an easy thing, as boys would think I am a loose girl. Parents at home were also closed up on us; now I think the knowledge which we are receiving in class will help me,” she said.
Both teachers and students in Zambia welcomed the introduction of CSE in schools and appreciate its contribution to the attitudes of young people.
“I saw the need to get more involved in teaching comprehensive sexuality education because of the way our society hides information on sexuality,” says Agather Shindende, a teacher at Kabulonga Primary School. “I remember growing up and being told that if you sit next to a boy at school you would conceive. I don’t want the current generation to go through what we went through.”
Schools have the potential to contribute to healthy individual behaviour as well as improved social norms around equality and non-violence, but this cannot be realized if, at the same time, they are places of gender inequality and violence. Access to a safe learning environment must be combined with education about gender equality, non-violent behaviour and sexual and reproductive health for everybody.
“Among the topics that I have learnt, gender stands out as the most interesting one,” says Harriet Lilanda. “I like gender because it teaches us to be equal. Boys and girls can do the same things—mathematics, science, home economics and technical drawing. I have learnt that we must respect each other and that household chores have to be done by girls and boys.”
Gender practices, norms and values influence sexuality, reproduction and relationships: unequal gender relations make it difficult for women and girls to make choices about sex, as well as increasing their vulnerability to violence, early marriage and adverse sexual and reproductive health outcomes.
Ms Shindende appreciates the benefits of CSE and feels that results are slowly being noticed. “The attitude and behaviour among learners regarding gender norms is slowly changing for the better, especially among boys,” she says. “Previously, boys never wanted to take subjects like home economics because they considered it as a subject for girls only, but today, out of 45 learners, 20 are boys and they willingly chose home economics as one of their optional subjects. Therefore, you can see that teaching comprehensive sexuality education from an early age can open up the minds of our young people. We also have many girls taking art and design courses, including technical drawing, which were exclusively for boys.”
When young women and adolescent girls have access to comprehensive age-appropriate sexuality education before becoming sexually active, they are more likely to make informed decisions about their sexuality and approach relationships with more self-confidence. CSE is also known to increase young girls’ condom use, increase voluntary HIV testing among young women and reduce adolescent pregnancy, especially when linked with non-school-based youth-friendly health services provided in a stigma-free environment.
Watch UNESCO video — Being a Young Person: Comprehensive Sexuality Education
Hands up for #HIVprevention — World AIDS Day campaign


Feature Story
Maximizing the potential of a new HIV prevention method: PrEP
01 November 2016
01 November 2016 01 November 2016Pre-exposure prophylaxis (PrEP)—most often a combination of tenofovir and emtricitabine taken orally as a daily tablet—is extremely effective at preventing HIV infection when taken regularly.
The choice of PrEP is recommended for people who are HIV-negative but at high risk of becoming infected. The people who can benefit most from PrEP—including gay men and other men who have sex with men, transgender people, sex workers, serodiscordant couples before the partner living with HIV becomes virally suppressed and young women and girls in the areas of sub-Saharan Africa most affected by HIV—are located where there are high rates of untreated HIV and inconsistent condom use.
People starting on PrEP must be HIV-negative and undergo repeat HIV testing every three months. The side-effects of taking PrEP are usually mild and short-lived. The risk of developing resistance to PrEP medicines is extremely low, as long as the person is confirmed to be HIV-negative when starting PrEP.
In the past two years, PrEP roll-out has moved quickly. It is estimated that in October 2016 around 100 000 people were using PrEP in more than 30 countries, with the majority of users in the United States of America. The UNAIDS target is for there to be 3 million people on PrEP worldwide by 2020.
There are now active national PrEP programmes in Australia, France, Kenya, Norway, South Africa and the United States. Botswana is pursuing regulatory approval and creating an implementation plan, while Thailand and Zimbabwe are among other countries producing guidelines for PrEP roll-out. In addition, more than 20 projects around the world are exploring the use of PrEP.
However, even where there is an existing national programme, PrEP uptake is unequal and the people who would benefit most do not always gain access. Many activists in the AIDS response continue to criticize this inequality. “PrEP is powerful, it has to reach the disempowered,” said Nöel Gordon of the Human Rights Campaign.
PrEP adds to the package of proven prevention options already available. PrEP should be used in conjunction with other prevention methods, such as male and female condoms, voluntary medical male circumcision and antiretroviral therapy for all people living with HIV. When antiretroviral therapy is effective in a person living with HIV, the virus becomes undetectable in the person’s blood and the risk of transmitting the virus to a partner approaches zero. No single HIV prevention method is 100% protective and PrEP does not prevent other sexually transmitted infections or prevent unintended pregnancy. Condoms remain the most widely available and affordable HIV prevention tool and as such should always be promoted along with PrEP.
The benefits of choosing PrEP can be psychological as well as physical and the use of PrEP may counter the anxiety and isolation felt by some people who feel they lack the ability to control their risk of exposure to HIV. PrEP can give people more autonomy about their sexual decision-making, which may also include risk reduction. PrEP may promote improved communication and intimacy with a partner, reduced fear of intimate partner violence, raised self-esteem and greater engagement with all aspects of sexual health.
Offering PrEP can encourage more people at the highest risk of HIV to attend HIV clinics, undergo HIV testing and access either PrEP or treatment depending on the test result. Either way, the outcome is good for the individual and good for HIV prevention.
PrEP gives us one more tool that we can use to better tailor the prevention package to each person’s individual needs, which can change over time. PrEP is not for everyone and is not for ever. Routine PrEP follow-up involves regular review of broader sexual health, including the diagnosis and treatment of sexually transmitted infections and discussion of appropriate combination HIV prevention strategies and contraception, as appropriate.
Hands up for #HIVprevention — World AIDS Day campaign




Feature Story
Ensuring HIV prevention and treatment services in Haiti are back on track after Hurricane Matthew
02 November 2016
02 November 2016 02 November 2016Haiti is regularly in the path of Atlantic Ocean storms, but Matthew was the most destructive hurricane in five decades and the country’s worst natural disaster since the devastating 2010 earthquake. According to the United Nations Office for the Coordination of Humanitarian Affairs, the hurricane killed 546 people, injured 438 and left thousands homeless. More than 141 000 displaced people are now living in temporary shelters.
Jasmin Désir, a community leader of the Union to Fight against Stigma and Discrimination, said the situation on the ground remains desperate for people with very few resources. It is even worse for many people living with HIV. He said their main concern now is being able to take antiretroviral medicines “when there is no food in sight.” Currently, 806 000 people need urgent food assistance.
Renel Julien, a community organizer living with HIV, mobilizes people living with HIV to get food and water. He thinks the emotional strain of dealing with the hurricane’s aftermath has taken a toll on many in the community.
Haiti’s entire health-care system was affected by the hurricane. Medical personnel and community health workers were unable to conduct home visits in some places. Most clinics were seriously damaged and some clinics and hospitals lost all their equipment, including generators, solar panels and computers. Antiretroviral medicines and other supplies were lost during the hurricane.
In the five most affected departments (Grand’Anse, South, South-East, Nippes and North-West), there were 13 994 people living with HIV and 37 functioning HIV treatment centres before Matthew.
According to UNAIDS Haiti, the hurricane has already affected HIV prevention, support, treatment and care services. Urgent programmes are needed to ensure that the current retention rate of people on treatment (between 60% and 80%) does not decline.
“One solution could be a community distribution system,” said Yafflo Ouattara, UNAIDS Country Director for Haiti. “In the short term, this might be the best option to reach people living with HIV who do not have access to their usual services.”
The UNAIDS country office in Haiti is currently supporting the national AIDS programme to gather information on the most affected departments and to explore alternatives for HIV treatment and care. Priorities include mapping treatment centres and reviewing the supply chain for antiretroviral medicines and other supplies.
Community leaders say marginalized groups, including gay men and other men who have sex with men, transgender people and sex workers, are even more vulnerable in these circumstances. Based on a preliminary assessment conducted by nongovernmental organizations in the areas most affected by the hurricane, stigma and discrimination has become a barrier to some people in need of assistance.
“Haiti was only just beginning the development phase to rebuild infrastructure following the 2010 earthquake that destroyed much of the country,” said Edner Boucicaut, Chair of Haiti’s Country Coordinating Mechanism for the Global Fund to Fight AIDS, Tuberculosis and Malaria and Country Director for Housing Works. “Having one disaster after another makes things more complicated than the typical emergency situation.”
César Núñez, Director of the UNAIDS Latin America and Caribbean Regional Support Team, said partners are working to ensure that the achievements made so far in the response to HIV are not diminished. “We are committed to ensuring that the excellent progress Haiti has made with respect to prevention and treatment is not reversed.”